The Clinical Roadmap of Oral Rehabilitation: Structuring the Treatment Pathway
Full mouth rehabilitation isn’t a single appointment. It’s a staged process sometimes spanning a year or more that works through the functional mechanics and aesthetic balance of the entire stomatognathic system in deliberate sequence. Clinics like Dentprime treat complex cases with exactly this kind of structured methodology, and there’s a good reason for it: you can’t bolt a final prosthetic onto a compromised foundation and expect it to last. Every phase sets up the next, and rushing any of them tends to cost more biologically and financially down the line.
Phase One: Diagnostic Precision and Digital Mapping
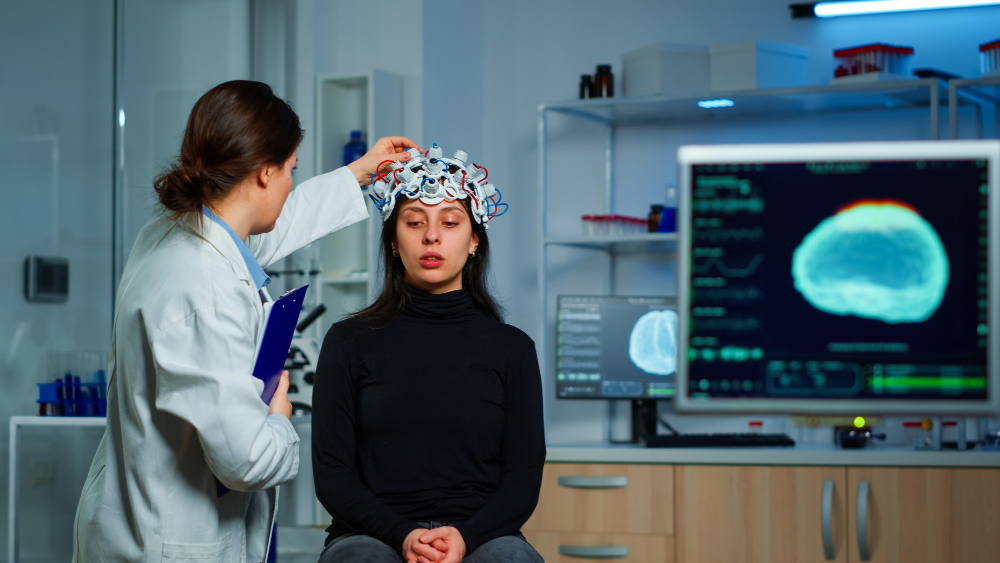
Before anything is cut, drilled, or designed, you need an accurate picture of what you’re actually working with. Modern clinical teams don’t rely on visual inspection alone anymore. Cone Beam Computed Tomography (CBCT) gives oral surgeons and prosthodontists a high-resolution, three-dimensional view of the maxillofacial structures alveolar bone density, the exact anatomical position of the inferior alveolar nerve, the volume of the maxillary sinus cavities. It’s the kind of data that makes surgical planning genuinely precise rather than approximate.
Pair that with digital intraoral scanners which generate accurate 3D models of the existing dentition and gingival architecture and you have enough information to build a treatment protocol tailored to the specific anatomy of one specific patient. No guesswork. No “we’ll deal with that when we get there.”
Phase Two: Establishing a Biologically Sound Foundation
Starting a dental journey without first stabilizing the biological environment is like repainting over rust. If infection, active gingival disease, or significant bone loss is already present, even well-fabricated prosthetics won’t hold.
This phase is often the least glamorous and the most important. Periodontal therapy comes first: eliminating active infections, clearing subgingival calculus, bringing localized inflammation under control. For patients who’ve experienced prolonged tooth loss, the alveolar bone may have resorbed to the point where implants simply don’t have enough volume to anchor into. In those cases, pre-prosthetic surgeries autogenous bone grafting, sinus augmentation are performed to rebuild that skeletal volume before anything else moves forward. Any teeth that can’t be saved get extracted here too, clearing the field for what comes next.
Phase Three: Surgical Execution and Structural Integration
With the oral environment stable, surgery begins. For edentulous or partially edentulous patients, this means placing endosseous implants biocompatible titanium roots inserted into prepared osteotomies under local anesthesia or IV sedation, torqued to precise specifications.
What happens after the surgery matters just as much as the surgery itself. Osseointegration the process by which living osteoblasts (bone-forming cells) mechanically interlock with the micro-textured titanium surface takes roughly three to six months. There’s no shortcut to that. The bone has to actually fuse with the implant for the fixture to be load-bearing long-term.
For patients pursuing smile design with porcelain veneers or crowns, this phase also involves the careful reduction of natural enamel and the capture of final digital impressions. Temporary acrylic restorations go in at this stage not just to protect exposed dentin, but to shape soft tissue contours and keep the aesthetic outcome consistent while the permanent restorations are being fabricated in the lab.
Phase Four: Prosthetic Fabrication and Biomechanical Alignment
The final restorations are where precision manufacturing takes over. High-end dental laboratories use CAD/CAM (Computer-Aided Design and Computer-Aided Manufacturing) technology to mill prosthetics from materials like monolithic zirconia or lithium disilicate chosen not just for their tensile strength and fracture resistance, but for their optical behavior. These materials replicate the natural translucency and light refraction of real tooth enamel in ways that earlier generations of ceramic simply couldn’t.
But fabricating a beautiful crown is only part of it. Placement is where things can quietly go wrong. The clinician has to evaluate occlusion the dynamic alignment of upper and lower teeth with real care. Even microscopic discrepancies in the bite pattern can distribute abnormal mechanical stress across the restorations. And that stress doesn’t stay confined to the ceramic; it can propagate into the temporomandibular joint, create muscular fatigue patterns, and, eventually, fracture the material itself. Getting the bite right isn’t a finishing touch it’s structural.
Phase Five: Post-Operative Maintenance and Biological Longevity
The last appointment isn’t the end of the process. It’s closer to the beginning of a different phase one that determines how long everything actually lasts.
Zirconia and titanium don’t decay. That part’s true. But the periodontal tissues and supporting bone around them are still fully biological, still vulnerable, still subject to bacterial infiltration. Peri-implantitis the progressive bone loss that develops around a neglected implant can undo months of surgical work surprisingly fast if oral hygiene slips. Patients need to commit to a daily routine that goes beyond a standard toothbrush: interdental brushes, water flossers, non-abrasive antimicrobial agents to disrupt biofilm before it establishes.
And twice-yearly clinical checkups aren’t optional. These visits allow the dental team to take radiographic measurements of bone levels, check soft tissue attachment, and confirm that occlusal forces are still balanced because the jaw does change over time, subtly, and what was perfectly calibrated at delivery might need adjustment two years later. Staying on top of that is how a full rehabilitation actually delivers on its long-term promise.